personality-tests
Big Five Personality and Mental Health Research
Discover how each Big Five personality trait predicts mental health outcomes, from neuroticism and depression risk to conscientiousness as a protective factor.
Quick answer
How do Big Five personality traits predict mental health?
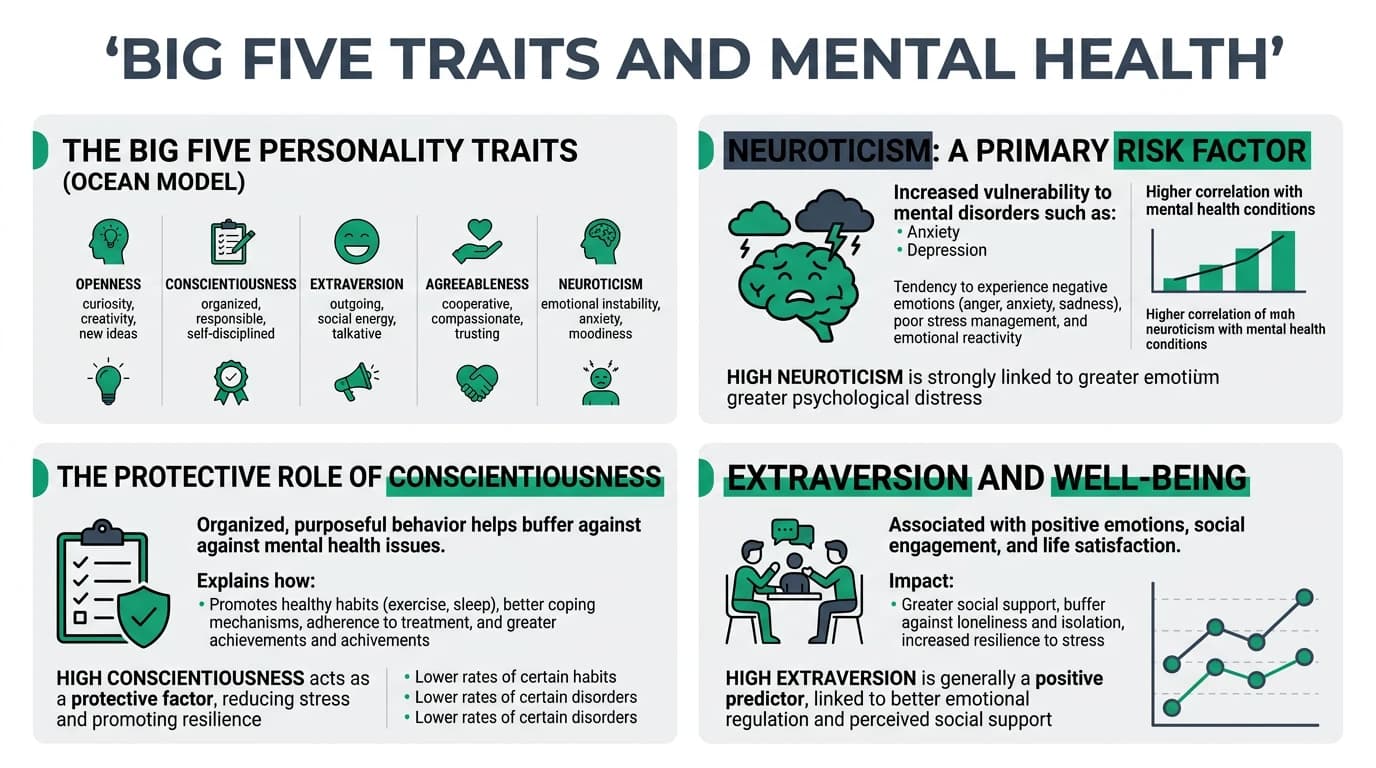
High neuroticism is the strongest personality predictor of anxiety, depression, and substance use disorders. Low conscientiousness predicts vulnerability across virtually all common mental disorders. Extraversion, agreeableness, and openness serve as protective factors through social support, reduced conflict, and adaptive coping strategies.
Key Takeaways
- Neuroticism is the most powerful personality predictor of mental health problems, with robust links to anxiety, depression, substance use, and personality disorders across 59 longitudinal studies1.
- Low conscientiousness predicts elevated risk for virtually all common mental disorders, including MDD, GAD, PTSD, panic disorder, and phobias (meta-analysis, n greater than 75,000)2.
- Extraversion protects against mood disorders through stronger social networks and positive emotion generation.
- Agreeableness buffers against depression and anxiety by reducing interpersonal conflict and strengthening social support.
- Openness shows balanced effects: creativity and adaptability support well-being, while elevated novelty-seeking can increase instability.
- Big Five traits outperform the MMPI for predicting borderline, avoidant, and dependent personality disorders2.
- Five distinct models (spectrum, vulnerability, scar, complication, and pathoplasty) explain the trait-mental health relationship, and they are not mutually exclusive2.
For the full framework of all five personality traits, see our complete Big Five personality test guide.
Disclaimer: This article summarizes personality and mental health research for educational purposes. It is not a substitute for professional psychological or psychiatric evaluation. If you are experiencing mental health concerns, consult a qualified healthcare provider.
The Big Five Framework and Mental Health
The Big Five model (OCEAN) provides a robust, empirically validated framework for understanding how personality traits interact with mental health outcomes. Decades of longitudinal research have established clear patterns linking specific trait profiles to both vulnerability and resilience.
| Trait | Primary Mental Health Role | Direction of Effect | Strength of Evidence |
|---|---|---|---|
| Neuroticism | Risk factor for most disorders | Higher N = higher risk | Very strong (59 longitudinal studies) |
| Conscientiousness | Protective against all common disorders | Lower C = higher risk | Strong (meta-analysis, n greater than 75,000) |
| Extraversion | Protective through social connection | Higher E = lower mood disorder risk | Strong |
| Agreeableness | Protective through reduced conflict | Higher A = lower anxiety and depression | Moderate to strong |
| Openness | Mixed: creativity protects, instability risks | Balanced effects | Moderate |
- The relationship between personality and mental health is bidirectional: traits predict disorder onset, and disorders can alter trait expression over time2.
- These findings hold after adjusting for baseline symptoms, psychiatric history, and demographic variables.
Neuroticism: The Primary Risk Factor
Neuroticism is the single most powerful personality predictor of mental health vulnerability. It captures emotional reactivity, stress sensitivity, and the tendency toward negative affect.
How Neuroticism Drives Mental Health Risk
- Emotional dysregulation: Difficulty managing negative emotions amplifies stress responses.
- Catastrophic thinking: Tendency to interpret ambiguous situations as threatening.
- Rumination: Repetitive focus on distressing thoughts without resolution.
- Heightened stress reactivity: Stronger physiological response to everyday stressors.
| Disorder | Effect of High Neuroticism | Effect Size | Key Citation |
|---|---|---|---|
| Generalized anxiety disorder | Strong predictor of onset and maintenance | Large | Lahey (2009)1 |
| Major depressive disorder | Predicts first episode and recurrence | Large | Kotov et al. (2010) meta-analysis3 |
| Panic disorder | Elevated risk through catastrophic body sensation interpretation | Moderate to large | Meta-analysis of 59 studies2 |
| Substance use disorders | Predicts onset through emotional coping motives | Moderate | Longitudinal predictions2 |
| Personality disorders | Elevated across borderline, avoidant, dependent PDs | Large | Big Five outperforms MMPI for prediction2 |
| PTSD | Predicts development after trauma exposure | Moderate | Longitudinal data2 |
| Neuroticism Level | Cognitive Pattern | Emotional Pattern | Behavioral Pattern |
|---|---|---|---|
| Very high (90th+ percentile) | Catastrophizing, hypervigilance | Frequent distress, emotional flooding | Avoidance, safety behaviors |
| High (70th-89th percentile) | Worry-prone, negative interpretation bias | Frequent anxiety, mood instability | Reassurance-seeking |
| Moderate (30th-69th percentile) | Balanced threat appraisal | Proportionate emotional responses | Adaptive coping |
| Low (below 30th percentile) | Optimistic, resilient appraisal | Emotional stability, calm under stress | Active problem-solving |
- Critical nuance: Not all high-neuroticism individuals develop disorders. Neuroticism creates vulnerability, but environmental triggers, social support, and coping strategies determine whether clinical conditions emerge1.
- High neuroticism paired with high conscientiousness partially buffers the risk through structured coping and self-regulation.
For strategies to manage neuroticism in professional settings, see our neuroticism workplace guide.
Conscientiousness: The Resilience Shield
Conscientiousness is the second most important Big Five trait for mental health, functioning as a broad protective factor across virtually all common disorders.
Protective Mechanisms
- Self-regulation: Controls impulses that lead to substance misuse and risky behavior.
- Structured coping: Approaches problems systematically rather than emotionally.
- Health behaviors: More consistent exercise, medication adherence, and sleep hygiene.
- Social stability: Maintains commitments that sustain relationships and support networks.
| Disorder | Effect of Low Conscientiousness | Sample Size / Evidence | Key Citation |
|---|---|---|---|
| Major depressive disorder | Strong risk factor | Meta-analysis, n greater than 75,000 | Kotov et al. (2010)3 |
| Generalized anxiety disorder | Moderate risk factor | Same meta-analysis | Kotov et al. (2010)3 |
| PTSD | Moderate risk factor | Longitudinal data | Multiple studies2 |
| Panic disorder | Moderate risk factor | Meta-analysis | Kotov et al. (2010)3 |
| Substance use disorders | Strong risk factor via impulse control | Longitudinal predictions | Roberts et al. (2007)4 |
| Social phobia | Moderate risk factor | Meta-analysis | Kotov et al. (2010)3 |
| Conscientiousness Facet | Mental Health Mechanism | Protective Effect |
|---|---|---|
| Self-discipline | Resists impulses toward harmful coping | Reduces substance use risk |
| Orderliness | Creates structure that reduces chaos-related stress | Lowers anxiety triggers |
| Dutifulness | Maintains therapy adherence and medication compliance | Improves treatment outcomes |
| Achievement striving | Provides purpose and goal-directed behavior | Buffers against depression |
| Deliberation | Prevents impulsive decisions during emotional distress | Reduces regret and self-blame |
| Competence | Maintains self-efficacy during challenges | Protects against learned helplessness |
- Low conscientiousness is the only trait (besides neuroticism) that consistently predicts elevated risk across all common mental disorders in the Kotov et al. (2010) meta-analysis3.
- Roberts et al. (2007) found that conscientiousness predicted longer lifespan, lower divorce rates, and reduced delinquency after controlling for other personality factors4.
Extraversion and Positive Mental Health
Extraversion protects against mood disorders primarily through social connection and positive emotion generation.
| Extraversion Level | Social Behavior | Mental Health Outcome | Mechanism |
|---|---|---|---|
| High | Engaged, outgoing, energized by others | Lower mood disorder risk | Strong social support, positive affect |
| Moderate | Selectively social, balanced energy | Generally stable | Adequate support, moderate stimulation |
| Low | Reserved, introspective, needs solitude | Higher risk of social isolation | Weaker informal support networks |
- High extraversion does not guarantee mental health, but it provides a structural advantage through broader social networks that offer emotional buffering during stress.
- Low extraversion is not inherently pathological. Introverts with strong, selective social connections and adequate solitary coping strategies can maintain excellent mental health.
- The risk emerges when low extraversion combines with high neuroticism and low agreeableness, creating social isolation with emotional vulnerability.
| Protective Factor | How Extraversion Helps | Clinical Implication |
|---|---|---|
| Social support access | More frequent, varied relationships | Faster access to help during crises |
| Positive emotion generation | Natural tendency toward enthusiasm | Buffers against depressive episodes |
| Activity engagement | Seeks stimulating experiences | Prevents withdrawal and rumination |
| Help-seeking behavior | Comfortable reaching out to others | Earlier intervention, better outcomes |
Agreeableness and Social Buffering
Agreeableness contributes to mental health through interpersonal harmony and social support quality rather than direct emotional regulation.
| Agreeableness Level | Social Impact | Mental Health Benefit | Risk |
|---|---|---|---|
| High | Strong, stable support networks | Lower anxiety and depression | People-pleasing burnout |
| Moderate | Balanced relationships | Generally stable | Minimal |
| Low | Potential for conflict, selective trust | Independent coping | Social isolation, hostility |
- High agreeableness reduces depression and anxiety risk primarily by creating environments with less interpersonal stress and more reliable emotional support3.
- In personality disorder research, low agreeableness (especially low trust and high antagonism) is the defining feature of antisocial, narcissistic, and paranoid personality pathology2.
- The combination of low agreeableness and high neuroticism is the most robust personality predictor of personality disorder diagnoses2.
Openness: Balanced Mental Health Effects
Openness to experience has the most nuanced relationship with mental health among the Big Five traits.
| Openness Aspect | Mental Health Effect | Mechanism |
|---|---|---|
| Creativity and imagination | Generally protective | Provides meaning, emotional expression |
| Intellectual curiosity | Protective | Engagement prevents stagnation |
| Novelty-seeking | Mixed | Adaptive exploration vs. instability |
| Emotional sensitivity | Mixed | Rich inner life vs. vulnerability to distress |
| Unconventionality | Mixed | Flexibility vs. rejection of helpful norms |
- High openness is associated with greater therapy engagement and willingness to explore psychological issues.
- The fantasy and feelings facets can increase vulnerability to emotional distress in individuals already prone to rumination.
- In dementia research (2023), higher openness predicted better adaptation to cognitive changes and greater quality of life post-diagnosis2.
Trait Predictions for Specific Disorders
Research allows precise mapping of Big Five trait profiles to specific mental health conditions.
| Disorder | Primary Risk Traits | Protective Traits | Prediction Accuracy | Key Evidence |
|---|---|---|---|---|
| Major depression | High N, Low C, Low E | High C, High E, High A | High | Meta-analysis, n greater than 75,0003 |
| Generalized anxiety | High N, Low C | High C, Moderate E | High | Lahey (2009)1 |
| PTSD | High N, Low C | High C, High A | Moderate | Longitudinal data2 |
| Social phobia | High N, Low E | High E, High A | Moderate to high | Multiple meta-analyses |
| Substance use disorders | High N, Low C, Low A | High C, High A | Moderate | Longitudinal predictions2 |
| Borderline PD | Very high N, Low A, Low C | High C, High A | High (outperforms MMPI) | Kotov et al. (2010)3 |
| Avoidant PD | Very high N, Low E | High E, Moderate A | High (outperforms MMPI) | Kotov et al. (2010)3 |
| Risk Profile | Trait Combination | Vulnerability Level | Recommended Focus |
|---|---|---|---|
| Highest risk | High N + Low C + Low A | Very high | Comprehensive intervention |
| High risk | High N + Low C | High | Structured coping and self-regulation |
| Moderate risk | High N + Average other traits | Moderate | Emotional regulation skills |
| Lower risk | Low N + High C | Low | Maintenance and prevention |
| Resilient | Low N + High C + High E + High A | Very low | Protective factors to maintain |
Trait Interaction Models
Five theoretical models explain how personality traits relate to mental health conditions. Crucially, these models are not mutually exclusive: different mechanisms may operate simultaneously for different traits and disorders2.
| Model | Core Idea | Example | Evidence Level |
|---|---|---|---|
| Spectrum | Disorder is an extreme of a normal trait | Neuroticism on a continuum with anxiety | Strong |
| Vulnerability | Trait predisposes to disorder onset | High N increases depression risk after stress | Strong |
| Scar | Disorder permanently alters trait levels | Depression episode increases neuroticism | Moderate |
| Complication | Disorder temporarily shifts trait expression | Acute anxiety elevates neuroticism scores | Moderate |
| Pathoplasty | Trait shapes disorder course without causing it | High C improves treatment adherence | Moderate to strong |
- The spectrum model has the strongest support for neuroticism-anxiety links, suggesting that clinical anxiety represents the extreme end of a normal personality dimension.
- The scar model explains why people who recover from depression often show lasting increases in neuroticism.
- The pathoplasty model has significant clinical utility: it explains why trait-informed treatment plans produce better outcomes without requiring that traits cause disorders.
Traits in Dementia and Cognitive Aging
Recent research (2023) has expanded the personality-mental health connection to dementia and cognitive aging, revealing important implications for quality of life.
| Trait | Effect When High | Effect When Low | Quality of Life Impact |
|---|---|---|---|
| Neuroticism | Greater psychological distress post-diagnosis | Better emotional adjustment | Strong negative effect when high |
| Conscientiousness | Better routine maintenance, medication adherence | Difficulty maintaining self-care | Moderate positive effect when high |
| Extraversion | Maintained social engagement | Social withdrawal risk | Moderate positive effect when high |
| Agreeableness | Cooperative with caregivers | Resistance to help | Moderate positive effect when high |
| Openness | Better adaptation to cognitive changes | Rigidity, frustration with limitations | Moderate positive effect when high |
- Pre-diagnosis personality profiles may help predict which individuals will adapt better to cognitive decline.
- Trait-informed caregiving strategies can significantly improve quality of life for dementia patients.
For insights on how personality traits change across the lifespan, see our personality changes guide.
Clinical Applications
Personality traits provide actionable guidance for personalizing mental health interventions.
| Trait Profile | Therapeutic Approach | Rationale | Expected Benefit |
|---|---|---|---|
| High neuroticism | CBT with emotional regulation focus | Addresses catastrophizing and rumination | Reduces anxiety and depression symptoms |
| Low conscientiousness | Structured behavioral activation | Provides external organization the individual lacks | Improves treatment adherence |
| Low extraversion | Gradual social exposure | Builds social support network | Reduces isolation risk |
| High agreeableness | Assertiveness training within therapy | Addresses people-pleasing and suppressed needs | Prevents burnout and resentment |
| High openness | Insight-oriented therapy | Leverages natural introspection and curiosity | Deeper therapeutic engagement |
- Trait-matched interventions produce better outcomes than one-size-fits-all approaches because they align treatment strategies with the patient's natural behavioral tendencies5.
- Emotional intelligence can be developed as a complementary skill, regardless of trait profile, to enhance resilience and coping capacity (Goleman, 2006)5.
For strategies to manage stress based on personality type, see our stress management guide.
For approaches to preventing burnout using Big Five awareness, see our burnout prevention guide.
Personality and mental health action checklist
- Take a validated Big Five assessment (IPIP-NEO is free) to identify your trait profile.
- If you score high in neuroticism, develop a structured emotional regulation practice (journaling, CBT techniques, mindfulness).
- If you score low in conscientiousness, build external systems for routine and self-care (alarms, checklists, accountability partners).
- Assess your social support network strength, especially if you score low in extraversion.
- Monitor for people-pleasing patterns if you score high in agreeableness.
- Discuss your trait profile with a mental health professional to personalize your treatment or prevention plan.
- Review your trait combination for known risk profiles (high N plus low C is highest risk).
- Reassess strategies quarterly and adjust based on life changes and stress levels.
FAQ
Is high neuroticism a mental health diagnosis?
No. Neuroticism is a personality trait, not a disorder. It describes a tendency toward emotional reactivity and negative affect. While high neuroticism increases vulnerability to clinical conditions like anxiety and depression, many high-neuroticism individuals never develop mental health disorders. The trait becomes clinically relevant when combined with environmental stressors and inadequate coping resources (Lahey, 2009)1.
Can personality traits predict which disorders someone will develop?
Yes, with meaningful accuracy. Meta-analyses show that specific trait profiles predict specific disorders: high neuroticism plus low conscientiousness predicts MDD, high neuroticism plus low extraversion predicts social phobia, and very high neuroticism plus low agreeableness predicts personality disorders. Big Five profiles outperform the MMPI for predicting borderline, avoidant, and dependent personality disorders (Kotov et al., 2010)3.
Does conscientiousness really protect against mental health problems?
Yes. Low conscientiousness is the only trait besides neuroticism that consistently predicts elevated risk across all common mental disorders in large meta-analyses (n greater than 75,000). The protective mechanism operates through self-regulation, structured coping, health behaviors, and social stability. Roberts et al. (2007) found that conscientiousness predicted longer life, lower divorce rates, and reduced delinquency even after controlling for other personality factors4.
Can personality traits change after a mental health episode?
Yes. The scar model proposes that mental health episodes can permanently alter trait levels. Research shows that depression episodes often increase neuroticism and decrease extraversion even after recovery. This creates a feedback loop where altered traits increase vulnerability to future episodes. However, effective treatment can mitigate these trait changes2.
How should therapists use Big Five information?
Therapists can use Big Five profiles to personalize treatment: CBT with emotional regulation for high neuroticism, behavioral activation for low conscientiousness, gradual social exposure for low extraversion, and assertiveness training for high agreeableness. The pathoplasty model suggests that traits shape treatment response without causing disorder, making trait-informed adjustment clinically valuable5.
Are introverts at higher risk for mental health problems?
Low extraversion alone is not a significant risk factor. The risk emerges when low extraversion combines with high neuroticism and low agreeableness, creating social isolation with emotional vulnerability. Introverts with strong selective relationships and adequate coping strategies show mental health outcomes comparable to extraverts. The key protective factor is social support quality, not quantity3.
What is the strongest personality predictor of depression?
High neuroticism is the strongest single predictor, but the combination of high neuroticism plus low conscientiousness plus low extraversion creates the most robust prediction. Kotov et al. (2010) found these three traits together predicted MDD with high accuracy across studies with over 75,000 participants3.
Can improving personality traits improve mental health?
Evidence supports this connection. Interventions that build conscientiousness (structured habits, planning skills), reduce neuroticism (CBT, mindfulness), or increase extraversion (social skills training) show corresponding mental health improvements. Personality traits are relatively stable but malleable, especially with sustained, targeted effort. The maturity principle shows natural trait improvement with age45.
Notes
Primary Sources
| Source | Type | Key Contribution | URL |
|---|---|---|---|
| APA - Journal of Personality and Social Psychology | Academic journal | Publishes foundational Big Five and mental health research | Link |
| PMC / NIH | Research database | Personality disorder models, longitudinal evidence, trait stability | Link |
| Simply Psychology | Educational reference | Big Five overview, trait descriptions, key meta-analysis summaries | Link |
| ScienceDirect | Research platform | Meta-analyses on neuroticism and mental health outcomes | Link |
Conclusion
The Big Five personality framework provides one of the most robust, empirically validated tools for understanding mental health vulnerability and resilience. Neuroticism and conscientiousness stand out as the two most clinically significant traits, with neuroticism as the strongest risk factor and conscientiousness as the broadest protective factor.
The practical implication is clear: personality awareness enables proactive mental health management. Knowing your trait profile allows you to anticipate vulnerabilities, build targeted coping strategies, and work with mental health professionals to personalize interventions.
Traits are not destiny. They represent tendencies that interact with environment, experience, and deliberate effort. The most effective approach combines trait awareness with evidence-based coping strategies and professional support when needed.
Footnotes
-
Lahey, B. B. (2009). Public health significance of neuroticism. American Psychologist, 64(4), 241-256. Overview: https://www.apa.org/pubs/journals/amp ↩ ↩2 ↩3 ↩4 ↩5 ↩6
-
Widiger, T. A. & Trull, T. J. (2007). Plate tectonics in the classification of personality disorder: Shifting to a dimensional model. American Psychologist, 62(2), 71-83. Referenced in PMC: https://pmc.ncbi.nlm.nih.gov/articles/PMC2730208/ ↩ ↩2 ↩3 ↩4 ↩5 ↩6 ↩7 ↩8 ↩9 ↩10 ↩11 ↩12 ↩13 ↩14 ↩15 ↩16 ↩17
-
Kotov, R., Gamez, W., Schmidt, F., & Watson, D. (2010). Linking "big" personality traits to anxiety, depressive, and substance use disorders: A meta-analysis. Psychological Bulletin, 136(5), 768-821. Published in: https://www.apa.org/pubs/journals/psp ↩ ↩2 ↩3 ↩4 ↩5 ↩6 ↩7 ↩8 ↩9 ↩10 ↩11 ↩12 ↩13
-
Roberts, B. W., Kuncel, N. R., Shiner, R., Caspi, A., & Goldberg, L. R. (2007). The power of personality: The comparative validity of personality traits, socioeconomic status, and cognitive ability for predicting important life outcomes. Perspectives on Psychological Science, 2(4), 313-345. ↩ ↩2 ↩3 ↩4
-
Goleman, D. (2006). Emotional Intelligence. Integration with Big Five discussed in: https://www.simplypsychology.org/big-five-personality.html ↩ ↩2 ↩3 ↩4